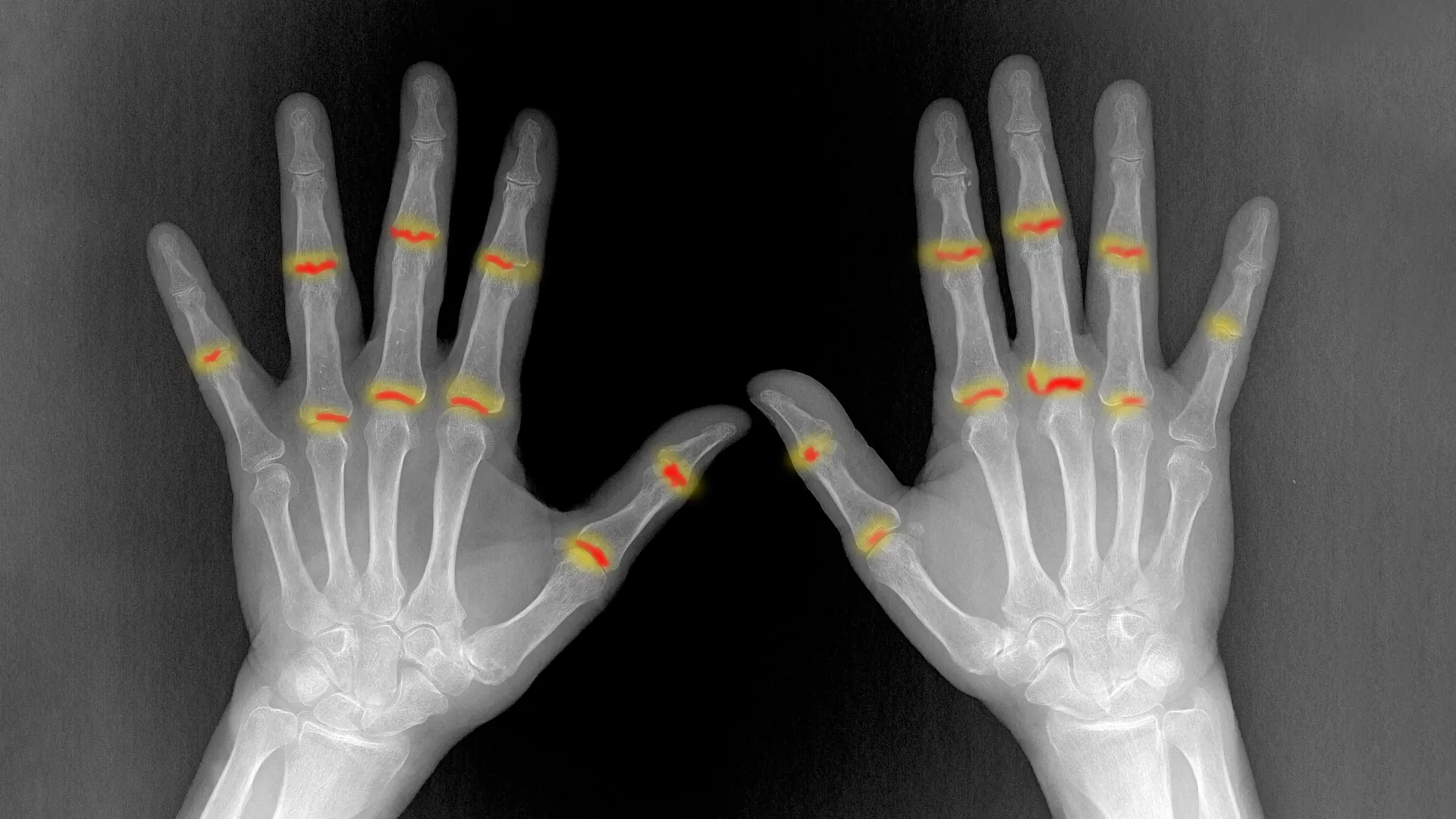
A significant proportion of individuals diagnosed with psoriasis, estimated between 20% and 30%, face the subsequent development of a debilitating inflammatory condition affecting their joints, known medically as psoriatic arthritis. This secondary ailment poses a serious threat, capable of inflicting irreversible damage to skeletal structures and articular tissues if left unaddressed. For an extended period, the precise mechanisms dictating why this progression occurs in a subset of psoriasis patients, while others remain unaffected, remained an enigma within the medical community.
However, a groundbreaking investigation conducted by a team of scientists affiliated with the Department of Medicine 3 – Rheumatology and Immunology at Uniklinikum Erlangen, part of the Friedrich-Alexander-Universität Erlangen-Nürnberg (FAU), has illuminated this complex interplay. Their work, published in the prestigious journal Nature Immunology, successfully identifies the specific types of immune cells instrumental in this transition and elucidates their journey from the dermal layers into the synovial joints. These revelations hold profound implications, suggesting novel avenues for the early detection and proactive prevention of psoriatic arthritis before irreversible joint deterioration takes hold.
The investigation delves into the intricate process by which immune cells, initially activated by the inflammatory milieu of psoriatic skin lesions, embark on a migratory path. These specialized immune precursor cells, generated in response to the chronic inflammation characteristic of psoriasis, are not confined to their origin tissue. The research indicates that these cells possess the capability to breach the dermal barrier and enter the systemic circulation. From the bloodstream, they are subsequently able to navigate towards and infiltrate the joints, initiating the cascade of events that can culminate in psoriatic arthritis.
Dr. Simon Rauber, who leads the investigative working group within Department of Medicine 3, emphasized this crucial migratory capability. "These cells possess the capacity to move from the skin into the bloodstream and subsequently reach the joints," he explained, underscoring the cellular exodus from affected skin. Yet, Dr. Rauber was quick to clarify that the mere presence of these migrating immune cells within the joint space is not inherently sufficient to provoke inflammation. This nuanced observation points to a critical secondary factor that determines the onset of psoriatic arthritis.
The pivotal determinant, according to the study’s findings, lies within the microenvironment of the joint itself and the interaction of these incoming immune cells with resident joint tissues. Specifically, the research highlights the role of fibroblasts, which are fundamental connective tissue cells normally tasked with maintaining the structural integrity and protective equilibrium of the joint. In individuals who ultimately develop psoriatic arthritis, the study reveals a significant impairment in the functional capacity of these fibroblasts.
Professor Dr. Andreas Ramming, a team leader and deputy head of the department, elaborated on this finding, stating, "The intrinsic protective function of these connective tissue cells is typically considerably compromised in individuals who subsequently develop psoriatic arthritis." This diminished protective capacity creates an environment where the infiltrating inflammatory cells are no longer effectively regulated or suppressed. Consequently, the unchecked inflammatory cells proceed to elicit a robust inflammatory response within the joint, thereby initiating the characteristic pathology of psoriatic arthritis. This intricate interplay between the migrating immune cells and the compromised joint environment provides a compelling explanation for the differential susceptibility observed among psoriasis patients.
Furthermore, the research team made a significant discovery regarding the potential for early detection. They identified that these migratory immune cells, the harbingers of potential joint inflammation, can be identified in peripheral blood samples even before the overt clinical manifestation of joint pain and swelling. This crucial finding opens the door to identifying individuals at heightened risk of developing psoriatic arthritis at a much earlier stage than previously possible.
The implications for future therapeutic strategies are substantial. The research suggests a paradigm shift towards interventions that target these specific immune cells proactively, potentially before they even reach the joints. By intercepting these inflammatory precursors or neutralizing their pathogenic potential in the systemic circulation, it may become feasible to prevent the onset of psoriatic arthritis altogether, rather than solely managing the damage after it has already occurred. This forward-looking approach could revolutionize the treatment and management of this complex condition, significantly improving patient outcomes and quality of life.
The scientific endeavor was supported by substantial funding from various prominent research bodies. The German Research Foundation (DFG) provided critical financial backing through its program focused on the "DIONE: Degeneration of bone due to inflammation" initiative. Additional support was secured from the European Research Council (ERC) as part of the "Barrier Break" project. Furthermore, the Interdisciplinary Center for Clinical Research in Erlangen (IZKF) contributed to the research through its project titled "Tissue imprinting of skin-derived immune cells in psoriatic arthritis," underscoring the collaborative and multi-faceted nature of this important scientific advancement.










