A groundbreaking investigation published in The Lancet Digital Health has unveiled a remarkable and counterintuitive adaptation within the human brain following a stroke, suggesting that even in the face of severe physical disability, certain neural regions can exhibit characteristics associated with younger biological age. This phenomenon, identified by researchers at the USC Mark and Mary Stevens Neuroimaging and Informatics Institute (Stevens INI), points to a profound capacity for the brain to reorganize and potentially rejuvenate undamaged networks as a compensatory mechanism for lost function. The study’s findings challenge traditional understandings of brain aging and recovery, offering a novel perspective on neuroplasticity through the lens of advanced artificial intelligence.
The extensive research effort, a significant component of the Enhancing NeuroImaging Genetics through Meta-Analysis (ENIGMA) Stroke Recovery Working Group, meticulously analyzed brain imaging data from an impressive cohort exceeding 500 individuals who had experienced a stroke. These scans, sourced from 34 distinct research centers spanning eight countries, represent a truly global dataset. By employing sophisticated deep learning algorithms, specifically trained on a vast repository of tens of thousands of magnetic resonance imaging (MRI) scans, the scientific team was able to estimate the biological age of various brain regions, both within the affected and unaffected hemispheres. This analysis allowed for a detailed examination of how stroke impacts brain structure and, crucially, how the brain responds and adapts during the recovery process, particularly in individuals with persistent physical limitations.
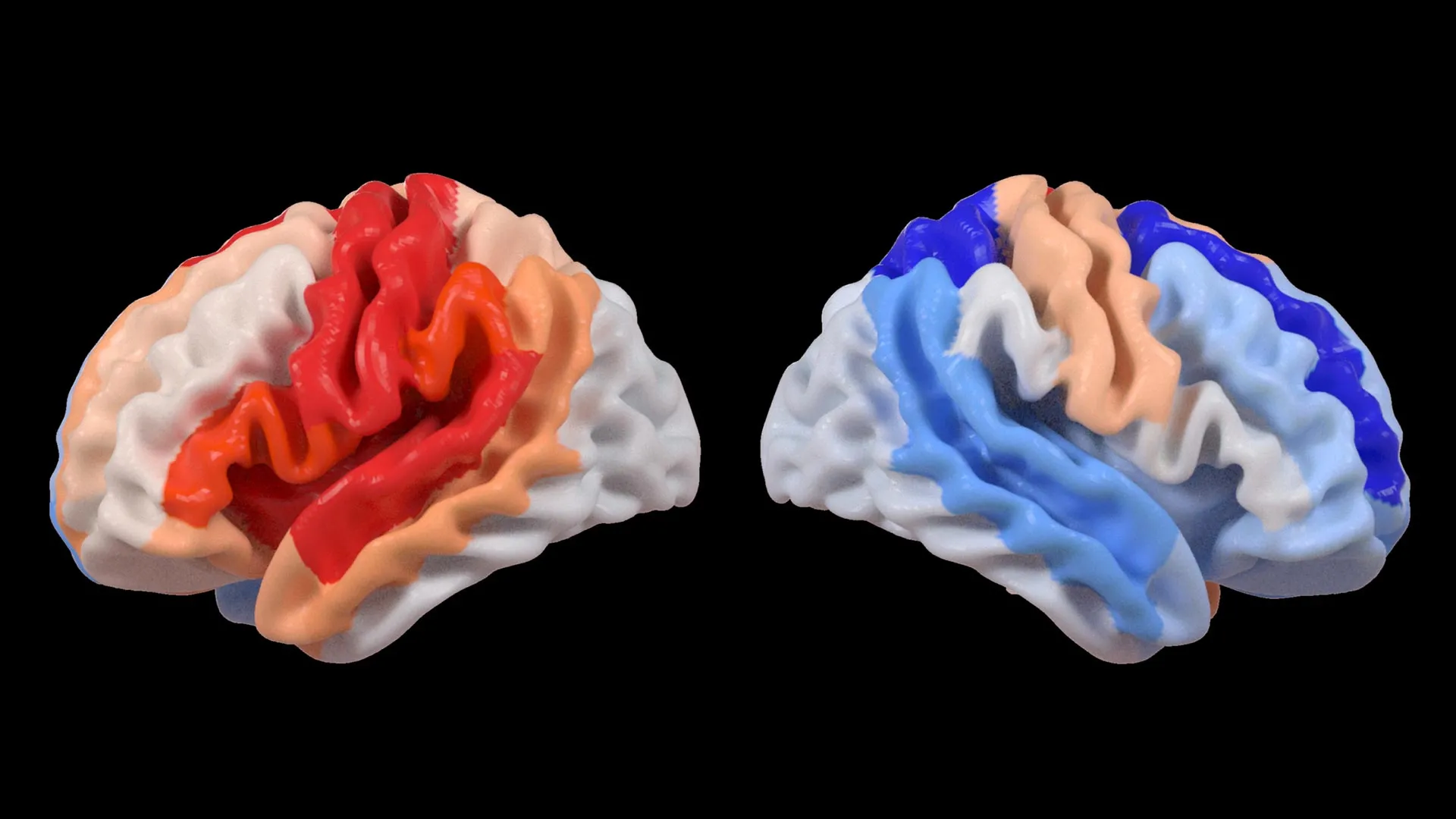
Hosung Kim, PhD, an associate professor of research neurology at the Keck School of Medicine of USC and a co-senior author of the study, articulated the central discovery with striking clarity. He observed that while substantial strokes demonstrably accelerate the aging process in the damaged hemisphere, a peculiar paradox emerges: the contralateral, or opposite, side of the brain appears to exhibit markers of reduced biological age. This pattern, Kim explained, strongly suggests an active process of brain reorganization, where undamaged neural pathways might be undergoing a form of rejuvenation to help offset the functional deficits caused by the stroke-induced injury. This implies that the brain is not merely passively enduring damage but is actively seeking strategies to maintain or regain functionality.
The sophisticated analytical framework underpinning this research utilized a specific form of artificial intelligence known as a graph convolutional network. This advanced AI system was instrumental in calculating the estimated biological age of 18 distinct brain regions based on the detailed anatomical information extracted from the MRI scans. This predicted brain age was then juxtaposed with each participant’s chronological age. The resultant metric, termed the brain-predicted age difference (brain-PAD), serves as a key indicator of brain health, with a negative brain-PAD generally signifying a younger-than-expected brain structure, and a positive brain-PAD indicating an older-than-expected structure.
A critical aspect of the study involved correlating these brain age estimations with quantitative measures of motor function. The results revealed a distinct and compelling pattern: stroke survivors who experienced significant motor impairments, even after undergoing more than six months of intensive rehabilitation, displayed a brain-PAD that was younger than anticipated in brain regions situated on the side opposite to the stroke’s origin. This effect was particularly pronounced within the frontoparietal network, a crucial neural circuit involved in complex cognitive functions such as the planning of movements, the allocation of attention, and the coordination of various bodily actions.
Dr. Kim further elaborated on the implications of this observation, suggesting that the increased youthfulness in these undamaged, contralateral regions might represent the brain’s adaptive response to compensate for the compromised motor system. He emphasized that the contralesional frontoparietal network, known for its role in motor planning and attentional processes, exhibiting a more "youthful" biological signature does not necessarily signify a complete restoration of motor function. Instead, it is more likely an indicator of the brain’s dynamic efforts to recalibrate and adjust when the primary motor pathways are no longer capable of operating effectively. This AI-driven approach, he noted, offers an unprecedented window into neuroplasticity that was previously beyond the capabilities of conventional neuroimaging techniques.
The sheer scale of the data employed in this research was pivotal in uncovering these subtle yet significant patterns. The study leveraged the infrastructure of ENIGMA, a vast international consortium dedicated to pooling brain imaging and clinical data from across more than 50 countries. This collaborative effort aims to foster a more comprehensive understanding of the human brain under a wide array of conditions. By meticulously standardizing MRI data and associated clinical information from numerous research groups, the team successfully assembled the most extensive stroke neuroimaging dataset of its kind to date, providing a robust foundation for advanced computational analysis.
Arthur W. Toga, PhD, director of the Stevens INI and Provost Professor at USC, highlighted the transformative power of this collaborative approach. He stated that by aggregating data from hundreds of stroke survivors worldwide and applying state-of-the-art artificial intelligence, researchers can now identify nuanced patterns of brain reorganization that would have remained undetectable in smaller, more localized studies. Toga expressed optimism that these insights into regionally differentiated brain aging in chronic stroke could ultimately pave the way for the development of more personalized and effective rehabilitation strategies tailored to the specific needs of individual patients.
Looking toward the future, the research team has outlined ambitious plans to extend this line of inquiry by longitudinally tracking patients from the acute phase following a stroke through their long-term recovery trajectories. By meticulously monitoring how patterns of brain aging and structural alterations evolve over time, clinicians may gain the ability to precisely customize therapeutic interventions for each person’s unique recovery pathway. The ultimate objective of this forward-looking research is to significantly improve patient outcomes and enhance their overall quality of life following a stroke.
The study, titled "Deep learning prediction of MRI-based regional brain age reveals contralesional neuroplasticity associated with severe motor impairment in chronic stroke: A worldwide ENIGMA study," received substantial financial support from the National Institutes of Health (NIH) under grant R01 NS115845. Further contributions and collaborative efforts were provided by international partners from esteemed institutions including the University of British Columbia, Monash University, Emory University, and the University of Oslo, underscoring the global and interdisciplinary nature of this important scientific endeavor. For those interested in exploring the association between contralesional neuroplasticity and motor impairment in greater detail, the Stevens INI has produced an informative video resource accessible online.









