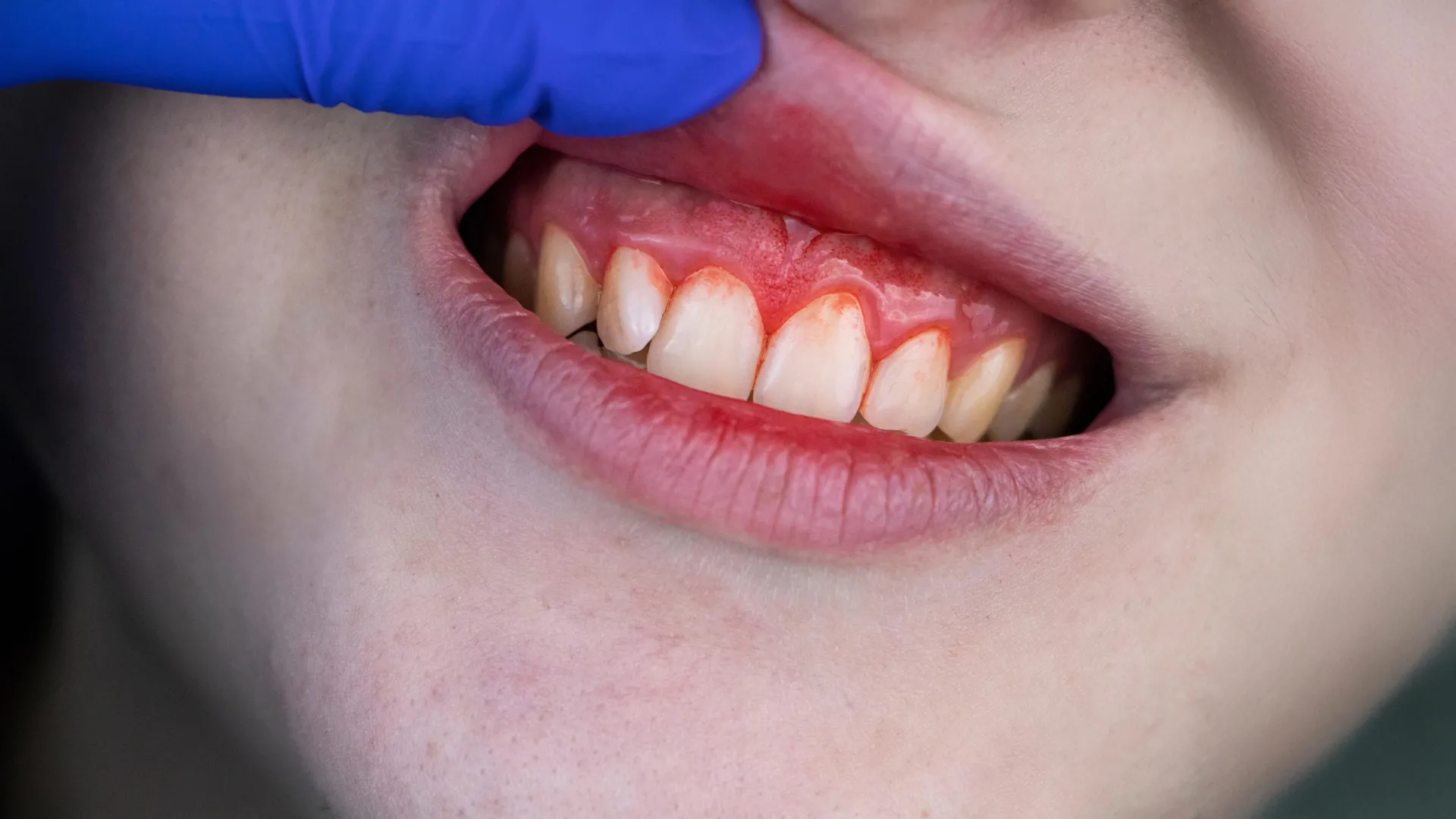
A recent comprehensive analysis of a significant national health dataset has illuminated a compelling link between dietary intake of lycopene, a vibrant pigment abundant in tomatoes and other red produce, and the severity of periodontal disease among older Americans. The investigation, which meticulously examined health and nutritional profiles of individuals aged 65 to 79, revealed that a substantial proportion of this demographic exhibits insufficient lycopene consumption, coinciding with an elevated predisposition to advanced gum inflammation. This groundbreaking research, meticulously detailed in the esteemed scientific publication The Journal of Nutrition, Health and Aging, was spearheaded by Katherine Kwong, an accomplished researcher affiliated with the Department of Human Development at Connecticut College, and involved a collaborative effort with esteemed scientists from a consortium of prominent academic institutions, including Tulane University, the University of California San Diego, Yunnan University, Southern Illinois University, and the Louisiana State University Health Sciences Center.
The study’s methodology involved a deep dive into the health and dietary information of 1,227 participants drawn from the National Health and Nutrition Examination Survey, a large-scale, ongoing data collection initiative spanning the years 2009 to 2014. The findings painted a stark picture: nearly half of the senior participants, specifically 48.7%, displayed observable indicators of periodontitis, a severe form of gum disease characterized by inflammation of the gums and deterioration of the bone and connective tissue that anchor teeth. Concurrently, a striking majority, amounting to 77.9% of the surveyed older adults, were found to be falling short of recommended daily lycopene intake levels. Lycopene, a potent antioxidant belonging to the carotenoid family, is most famously recognized for imparting the characteristic red hue to fruits like tomatoes, watermelons, and grapefruits, and is also present in smaller quantities in other fruits and vegetables. Its well-documented antioxidant properties have long been a subject of scientific inquiry, with research exploring its potential roles in mitigating oxidative stress and inflammation throughout the body.
Upon statistically adjusting for a multifaceted array of potential confounding variables—including chronological age, biological sex, racial and ethnic background, established smoking behaviors, and educational attainment—the researchers identified a robust and statistically significant inverse correlation between lycopene consumption and the prevalence and severity of gum disease. Specifically, older adults who consistently met the established guidelines for lycopene intake demonstrated a markedly lower likelihood of experiencing severe periodontitis. Their odds of developing this advanced stage of gum disease were approximately one-third when compared to their counterparts whose dietary habits resulted in insufficient lycopene levels. This suggests that lycopene may play a protective role, potentially by modulating inflammatory pathways or bolstering the integrity of oral tissues, thereby offering a degree of resilience against the destructive processes of periodontal disease.
Beyond the overarching association between lycopene and gum health, the study’s granular analysis also brought to light significant and concerning disparities in the prevalence of severe periodontitis across different demographic segments of the older American population. The data indicated that men, as a group, exhibited a higher incidence of severe gum disease compared to women. Furthermore, non-Hispanic Black adults were disproportionately affected, presenting with more frequent occurrences of advanced periodontitis than other racial and ethnic groups within the study cohort. These observed differences underscore the complex interplay of biological, environmental, and socioeconomic factors that contribute to health outcomes, highlighting the need for targeted public health interventions and further research to understand the root causes of these disparities.
The implications of these findings, as articulated by the study’s authors, point towards dietary lycopene as a potentially modifiable factor that could be leveraged in strategies aimed at preventing severe gum disease among the aging population. However, the researchers were careful to emphasize the inherent limitations of the study’s cross-sectional design. This type of observational study, while excellent for identifying associations, cannot definitively establish a cause-and-effect relationship. In simpler terms, while the data strongly suggest that low lycopene intake is linked to a higher risk of severe gum disease, it does not definitively prove that insufficient lycopene is the direct cause. Other unmeasured factors or a complex web of interactions could be at play.
Consequently, the research team underscored the critical importance of further scientific investigation to solidify these findings and explore potential therapeutic avenues. They strongly advocate for longitudinal studies, which track individuals over extended periods, and randomized controlled trials, considered the gold standard for establishing causality, to ascertain whether actively increasing lycopene consumption can indeed lead to a tangible reduction in the risk of developing severe gum disease or effectively slow its progression in individuals already affected. Such studies would involve carefully controlled interventions, such as dietary supplementation or specific dietary guidance, to measure the impact on periodontal health outcomes.
Moreover, the researchers drew attention to the broader public health concern represented by the racial and sex-based disparities identified in periodontal disease prevalence. The consistent observation that non-Hispanic Black adults and men experience higher rates of severe gum disease necessitates a more nuanced and targeted approach to oral health promotion and disease prevention. Future public health initiatives and clinical guidelines should actively incorporate an awareness of these demographic differences, tailoring interventions and educational materials to address the specific needs and risk factors prevalent within these vulnerable groups. This could involve culturally sensitive outreach programs, targeted screenings, and educational campaigns that resonate with the lived experiences and health beliefs of these communities. Understanding and addressing these disparities is not only a matter of scientific rigor but also a crucial step towards achieving greater health equity.










