A comprehensive re-evaluation of existing data by researchers at University College London (UCL) has dramatically reshaped our understanding of Alzheimer’s disease, suggesting that a single gene, APOE, may be the principal driver behind a vast majority of cases. This groundbreaking analysis posits that upwards of 90% of Alzheimer’s diagnoses might not materialize in the absence of this critical gene’s influence. The ramifications of this discovery extend beyond Alzheimer’s, with the study indicating that nearly half of all dementia cases globally could also be intricately linked to APOE’s function.
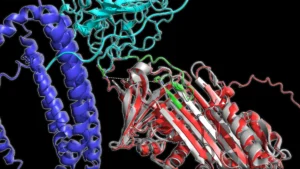
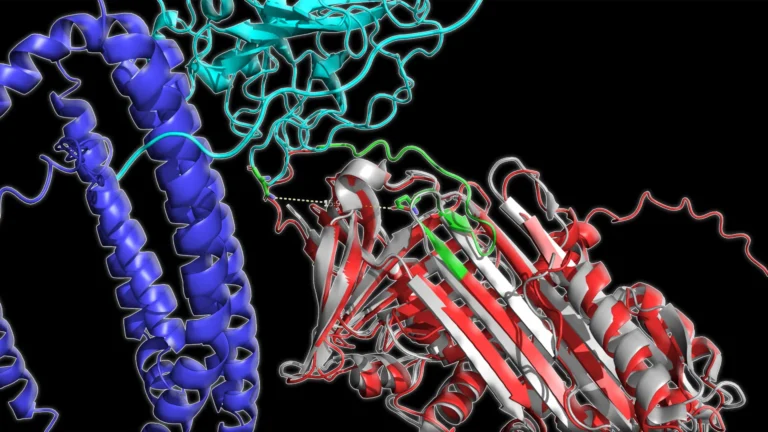
The findings, meticulously detailed in the journal npj Dementia, highlight the protein produced by the APOE gene as a paramount, yet historically underemphasized, target for the development of novel therapeutic interventions. By focusing efforts on this gene and its associated pathways, scientists may unlock avenues for preventing or effectively treating a substantial proportion of neurodegenerative diseases that afflict millions worldwide. This shift in perspective could redefine the landscape of dementia research and drug discovery.
For decades, the scientific community has acknowledged a connection between the APOE gene and an increased susceptibility to Alzheimer’s disease. This gene exists in three primary common forms, or alleles: APOE2, APOE3, and APOE4. Each individual inherits two copies of the APOE gene, leading to six possible combinations of these variants. Early research, dating back to the 1990s, established a clear correlation: individuals carrying one or two copies of the APOE4 variant face a significantly elevated risk of developing Alzheimer’s compared to those who inherit two copies of the APOE3 variant. Conversely, possessing APOE2 has generally been associated with a reduced risk compared to APOE3 carriers.
However, the recent UCL-led analysis challenges the prevailing view that APOE’s contribution has been fully appreciated, particularly concerning the APOE3 allele. Dr. Dylan Williams, the study’s lead author from UCL’s Division of Psychiatry and Unit for Lifelong Health and Ageing, articulated this crucial insight: "We have long underestimated how much the APOE gene contributes to the burden of Alzheimer’s disease. The ε4 variant of APOE is well recognized as harmful by dementia researchers, but much disease would not occur without the additional impact of the common ε3 allele, which has been typically misperceived as neutral in terms of Alzheimer’s risk." This re-evaluation suggests that the seemingly innocuous APOE3 allele, which is the most common form, plays a far more significant role in disease development than previously assumed.
Dr. Williams elaborated on the implications of considering both APOE3 and APOE4: "When we consider the contributions of ε3 and ε4, we can see that APOE potentially has a role in almost all Alzheimer’s disease. Consequently, if we knew how to reduce the risk that the ε3 and ε4 variants confer to people, we may be able prevent most disease from occurring." This statement underscores the potential for widespread impact if interventions targeting these common APOE variants can be developed.
This extensive investigation represents the most ambitious modeling study to date, aiming to quantify the population-level impact of common APOE variants on Alzheimer’s and dementia incidence. The research team meticulously synthesized evidence that links APOE3 and APOE4 to Alzheimer’s diagnoses, broader dementia classifications, and the subtle, preclinical changes observed in brain tissue that often precede overt symptoms. A significant methodological strength of this analysis was its access to aggregated data from four large-scale studies, encompassing over 450,000 participants. This substantial dataset facilitated the identification of a sufficiently large cohort of individuals with two APOE2 copies – an uncommon but low-risk group – who served as a crucial baseline for comparative analysis, a practice rarely implemented in previous studies of this nature.
Through this rigorous approach, the researchers calculated that between 72% and 93% of Alzheimer’s cases might have been averted had the APOE3 and APOE4 variants not been present. Furthermore, the study concluded that approximately 45% of all dementia cases could be attributed to the influence of the APOE gene. These figures represent a considerable upward revision of earlier estimates concerning APOE’s contribution, primarily due to the inclusion of APOE3’s effects alongside APOE4, rather than solely focusing on the latter.
The variations observed in the results across the four constituent studies underscore the inherent complexities in defining and diagnosing Alzheimer’s and other forms of dementia. Differences in diagnostic criteria, measurement methodologies – whether relying on medical records, established dementia classifications, or advanced imaging techniques like amyloid PET scans – and variations in participant follow-up periods and recruitment strategies all contributed to the observed discrepancies. Nevertheless, when viewed collectively, the accumulated evidence strongly suggests that APOE is responsible for at least three-quarters of Alzheimer’s cases, with the potential to account for an even greater proportion.
These findings carry profound implications for the future direction of drug development and preventive strategies. The study advocates for elevating APOE to a higher priority within research endeavors focused on unraveling disease mechanisms and devising innovative treatments. Dr. Williams emphasized the burgeoning field of gene editing and therapy, stating, "There has been major progress in recent years in gene editing and other forms of gene therapy to target genetic risk factors directly. Moreover, genetic risk also points us towards parts of our physiology that we could target with more conventional drugs." He further noted the potential for interventions that directly address the APOE gene or the molecular pathways linking it to disease, suggesting that such approaches could hold "great, and probably under-appreciated, potential for preventing or treating a large majority of Alzheimer’s disease." This sentiment highlights a perceived gap between APOE’s genetic importance and its historical representation in therapeutic research: "The extent to which APOE has been researched in relation to Alzheimer’s or as a drug target has clearly not been proportionate to its full importance."
While the genetic predisposition conferred by APOE is undeniably powerful, it is crucial to recognize that it is not the sole determinant of Alzheimer’s or other dementias. Even individuals with the highest genetic risk, such as those carrying two APOE4 copies, do not face a 100% lifetime probability of developing the disease; their risk typically remains below 70%. This observation underscores the intricate interplay of various factors. Dr. Williams explained this complexity: "Most people with genetic risk factors like APOE ε3 and ε4 won’t get dementia in a typical lifetime, since there are complicated interactions at play with other contributing genetic and environmental risk factors. Understanding what modifies the risk people inherit from their APOE genes is another crucial question for dementia researchers to grapple with."
This perspective aligns with broader public health initiatives focused on dementia prevention. Emerging research, such as the 2024 Lancet Commission report, suggests that a significant portion of dementia cases – potentially as much as half – could be prevented or delayed through the management of modifiable risk factors, including social isolation, high cholesterol, and smoking. The multi-faceted nature of Alzheimer’s and other dementias implies that multiple avenues for risk reduction should be explored. "With complex diseases like Alzheimer’s and other diseases that cause dementia, there will be more than one way to reduce disease occurrence. We should explore many options by which we might modify Alzheimer’s and dementia risk, including but not limited to strategies related to APOE," Dr. Williams stated. He reiterated the central finding of the current study: "Nonetheless, we should not overlook the fact that without the contributions of APOE ε3 and ε4, most Alzheimer’s disease cases would not occur, irrespective of what other factors are inherited or experienced by carriers of these variants throughout life."
The research was a collaborative effort between UCL and the University of Eastern Finland, receiving financial support from organizations such as Alzheimer’s Research UK and the Medical Research Council. Dr. Sheona Scales, Director of Research at Alzheimer’s Research UK, commented on the study’s significance, noting, "This study highlights that more Alzheimer’s cases are linked to the APOE gene that previously thought. However, not everyone with these variants will develop Alzheimer’s, demonstrating the complex relationship between genetics and other risk factors for dementia." She echoed the call for increased focus on APOE in therapeutic development: "Despite APOE being linked to Alzheimer’s, very few treatments in clinical trials target this gene directly. Findings from this study show that further research into APOE will be important for developing future prevention and treatment strategies for Alzheimer’s." Alzheimer’s Research UK expressed enthusiasm for supporting Dr. Williams’ ongoing work in this critical area, aiming to advance the understanding of how genetic, environmental, and societal factors converge to influence dementia risk, ultimately bringing the scientific community closer to a cure.
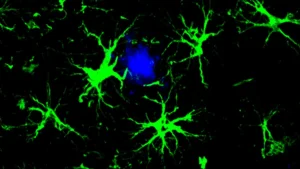
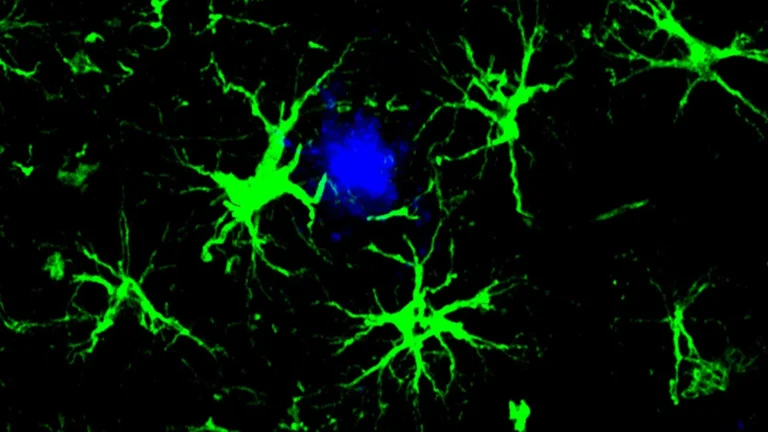
The precise mechanisms by which APOE variants increase dementia risk are still under investigation, but existing research offers potential explanations. The APOE4 variant, for instance, is thought to impair the protein’s ability to clear amyloid-beta, a sticky protein that aggregates into plaques in the brain, a hallmark of Alzheimer’s disease. Furthermore, APOE4 may disrupt the way brain cells manage lipids and energy, and promote neuroinflammation, processes that can incrementally damage neurons and heighten vulnerability to neurodegenerative conditions. Further research is imperative to definitively confirm these pathways and to elucidate why APOE3, compared to APOE2, also appears to confer an increased dementia risk.