A comprehensive investigation spearheaded by researchers at the University of Cambridge has illuminated significant associations between the menopausal transition and observable alterations in brain structure, alongside a heightened prevalence of psychological distress and sleep disturbances. The study’s findings indicate a discernible reduction in grey matter volume within critical brain areas among women who have concluded their reproductive years. This neurobiological impact appears to coincide with an increased susceptibility to conditions such as anxiety, depression, and disrupted sleep patterns, presenting a multifaceted challenge for women navigating this life stage.
The research, detailed in the esteemed journal Psychological Medicine, also delved into the complex interplay between hormone replacement therapy (HRT) and these menopausal effects. While the administration of HRT did not demonstrate a capacity to fully counteract the observed structural brain changes or the attendant mental health detriments, it was nonetheless correlated with a deceleration in the decline of reaction speed, suggesting a nuanced protective role in certain cognitive domains.
Menopause, a natural biological process, signifies the definitive cessation of menstruation, a consequence of the natural decline in ovarian hormone production. This pivotal life event typically unfolds between the ages of 45 and 55 and is frequently accompanied by a spectrum of somatic and psychological symptoms. These can range from intensely uncomfortable hot flashes and mood fluctuations to significant disruptions in sleep architecture. A growing body of scientific literature has already established a connection between menopause and alterations in cognitive faculties, impacting domains such as memory recall, attentional capacity, and language processing.
To address and alleviate the often-debilitating symptoms associated with menopause, particularly depression and sleep disturbances, many women are prescribed HRT. The adoption of HRT is substantial, with a notable percentage of women in countries like England utilizing it in recent years, reflecting its perceived efficacy in managing menopausal symptoms. Despite its widespread application, a comprehensive understanding of how menopause and HRT specifically influence the intricate architecture of the brain, the nuances of cognitive processing, and overall mental health remains an active area of scientific inquiry.
To meticulously examine these effects, the Cambridge research team undertook an extensive analysis of data sourced from the UK Biobank, encompassing the participation of nearly 125,000 women. The cohort was strategically segmented into three distinct groups to facilitate comparative analysis: women who had not yet experienced menopause, women who were post-menopausal and had never undergone HRT, and women who were post-menopausal and had previously or were currently utilizing HRT. This stratification allowed for a nuanced exploration of the independent and potentially interacting effects of menopausal status and HRT.
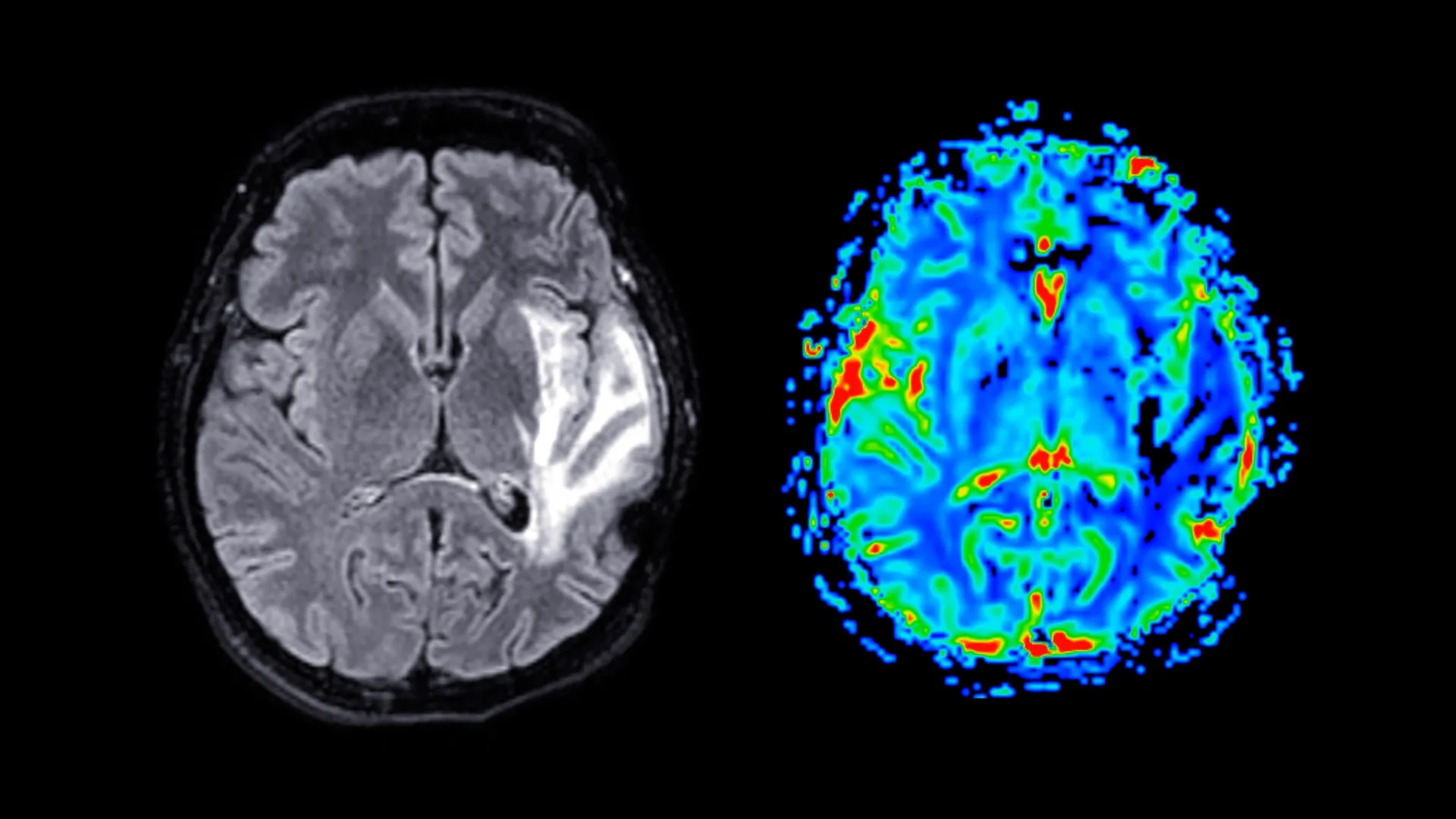
Participants were invited to complete a series of detailed questionnaires designed to capture information pertaining to menopausal symptoms, their psychological well-being, established sleep patterns, and their general health status. A subset of these participants also engaged in a battery of cognitive assessments, meticulously designed to evaluate their memory retention capabilities and their speed of response. Furthermore, approximately 11,000 women underwent advanced magnetic resonance imaging (MRI) scans, a non-invasive neuroimaging technique that provided researchers with high-resolution insights into the structural characteristics of their brains, enabling the detection of subtle variations in volume and organization. The average age at which participants reached menopause was approximately 49.5 years, with those prescribed HRT typically initiating treatment around the age of 49, underscoring the proximity of HRT initiation to the menopausal transition itself.
The findings revealed a significant disparity in mental health reporting between menopausal and pre-menopausal women. Post-menopausal women demonstrated a greater propensity to seek medical attention from general practitioners or psychiatrists for symptoms of anxiety, nervousness, or depression when contrasted with their pre-menopausal counterparts. This clinical observation was further substantiated by higher scores on validated depression questionnaires and a greater likelihood of having been prescribed antidepressant medications among the post-menopausal cohort. Interestingly, women in the HRT group exhibited higher reported levels of anxiety and depression when compared to women who had not used HRT. However, a deeper dive into the data suggested that these pre-existing mental health challenges may have influenced HRT prescription decisions. The researchers posited that some physicians might have prescribed HRT proactively, anticipating that the onset of menopause could exacerbate pre-existing psychological vulnerabilities.
Sleep disturbances emerged as another prevalent issue following menopause. Post-menopausal women were more inclined to report experiencing insomnia, reduced overall sleep duration, and persistent feelings of daytime fatigue. Intriguingly, women undergoing HRT reported experiencing the most profound fatigue, even though their measured total sleep duration did not significantly differ from that of post-menopausal women not receiving HRT, suggesting a potential qualitative difference in their sleep experience or other contributing factors.
The importance of holistic well-being during this transitional period was underscored by expert commentary. Dr. Christelle Langley from the Department of Psychiatry emphasized that menopause is a profound life transition for most women, irrespective of their HRT status. She highlighted the critical role of adopting a healthy lifestyle, which includes regular physical activity and a balanced diet, as an essential strategy for mitigating some of the adverse effects associated with this phase of life. Dr. Langley also advocated for increased societal and clinical sensitivity towards both the physical and mental health needs of women during menopause, stressing the importance of recognizing when individuals are struggling and destigmatizing the act of seeking support.
In terms of cognitive performance, menopause was associated with observable changes. Women who were post-menopausal and not utilizing HRT exhibited a noticeable slowing in their reaction times when compared to both pre-menopausal women and those undergoing HRT. This effect suggests that the absence of HRT during the post-menopausal period might contribute to a more pronounced decline in processing speed. Crucially, memory performance did not show significant divergence across the three groups, indicating that while the speed of cognitive processing may be affected, the fundamental capacity for memory formation and retrieval remained largely intact.
Dr. Katharina Zühlsdorff from the Department of Psychology at the University of Cambridge provided a comparative perspective, noting that a general slowing of reaction times is an intrinsic aspect of the natural aging process, affecting both men and women. She likened this to the speed at which individuals might retrieve information, where younger individuals would likely respond more rapidly. Dr. Zühlsdorff suggested that menopause appears to accelerate this age-related slowing of reaction times, whereas HRT, conversely, seems to exert a moderating influence, potentially slowing down this aspect of the aging trajectory.
The neuroimaging component of the study yielded significant insights into structural brain changes. Magnetic resonance imaging revealed that post-menopausal women exhibited substantial reductions in grey matter volume, a finding that held true regardless of their HRT usage. Grey matter, the densely packed region of the brain composed primarily of neuronal cell bodies, is fundamental to a wide array of cognitive functions, including information processing, motor control, memory consolidation, and the intricate regulation of emotions. The most pronounced reductions in grey matter were observed in key brain regions: the hippocampus, a structure critically involved in the formation and storage of new memories; the entorhinal cortex, which serves as a vital conduit for information transfer between the hippocampus and other brain areas; and the anterior cingulate cortex, a region implicated in executive functions such as emotional management, decision-making, and focused attention.
The identification of these affected brain regions carries potentially significant implications for understanding women’s long-term neurological health. Professor Barbara Sahakian, the senior author of the study from the Department of Psychiatry, highlighted that the brain areas exhibiting these structural differences are precisely those that are typically impacted by Alzheimer’s disease. This observation leads to the hypothesis that menopause could render women more susceptible to neurodegenerative conditions later in life. While acknowledging that this is not the sole determinant, Professor Sahakian proposed that these menopausal-induced brain changes might contribute to the observed epidemiological phenomenon of nearly twice as many dementia cases occurring in women compared to men, suggesting a potential link between the menopausal transition and increased vulnerability to cognitive decline and dementia.








