The global health landscape continues to grapple with the pervasive challenge of obesity, a chronic and complex disease affecting hundreds of millions worldwide. With its significant comorbidities, including type 2 diabetes, cardiovascular disease, and certain cancers, the search for effective interventions remains a critical public health priority. In recent years, a class of medications known as GLP-1 receptor agonists, exemplified by semaglutide, has revolutionized weight management and diabetes treatment. While initially available primarily through injectable formulations, the advent of oral alternatives has marked a pivotal shift, promising enhanced patient convenience and adherence. However, a recent investigation from the University of Adelaide suggests that the seemingly inert components enabling these oral therapies may exert biological influences extending beyond their primary function, prompting a call for more exhaustive long-term evaluations.
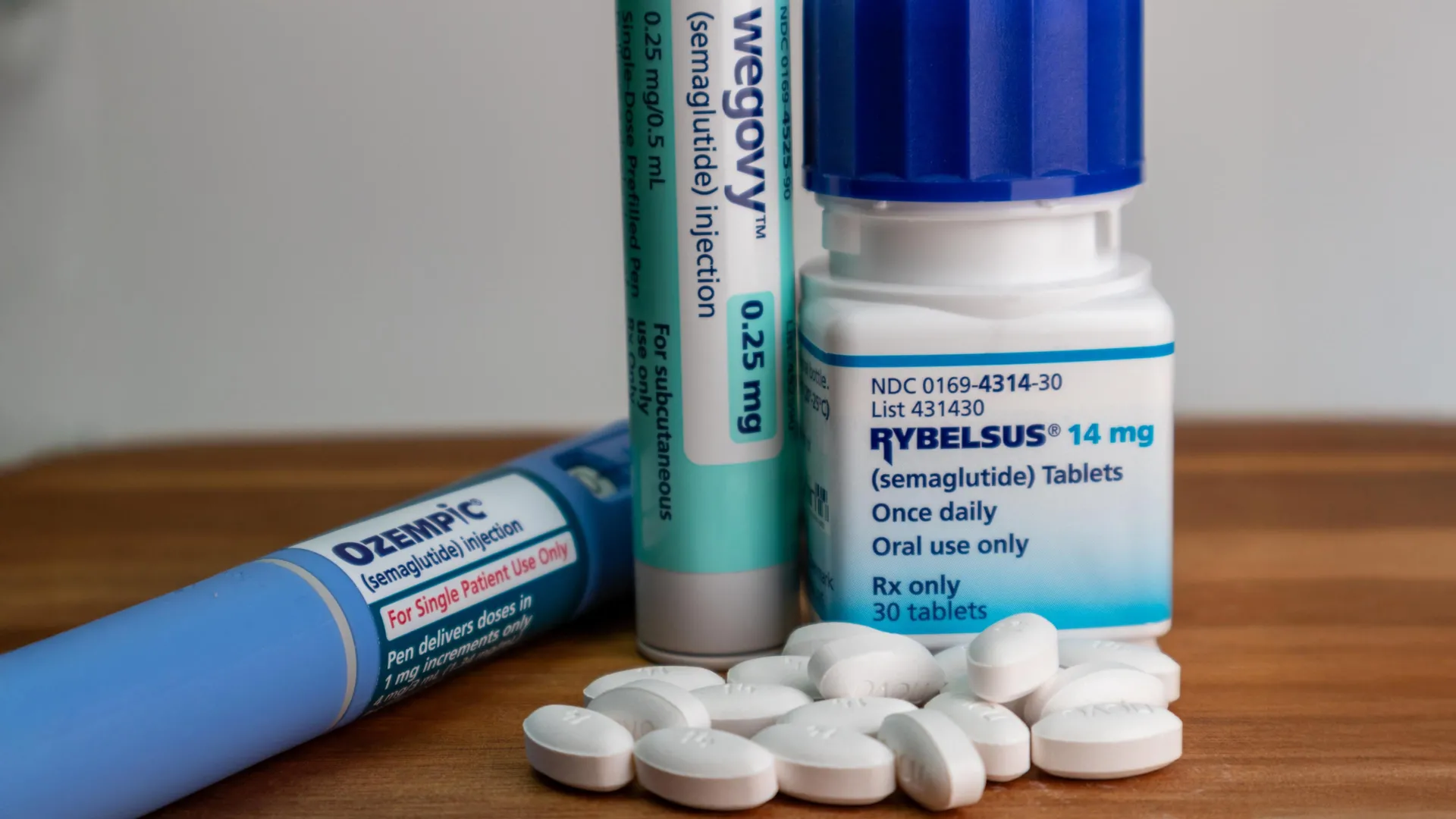
Semaglutide, the active pharmaceutical ingredient in popular medications such as Ozempic and Wegovy, works by mimicking the action of glucagon-like peptide-1 (GLP-1), a hormone that regulates blood sugar, slows gastric emptying, and promotes satiety. These mechanisms contribute significantly to weight reduction and improved glycemic control. Historically, peptide-based drugs like semaglutide faced substantial hurdles for oral administration. The harsh acidic environment of the stomach and the presence of proteolytic enzymes rapidly degrade these delicate molecules, rendering them ineffective before they can reach the bloodstream. Furthermore, the large size of peptide molecules makes their absorption across the intestinal lining inherently challenging.
To overcome these bioavailability obstacles, pharmaceutical scientists developed innovative delivery systems. For oral semaglutide, this breakthrough came in the form of salcaprozate sodium, commonly known as SNAC. SNAC functions as a permeability enhancer, a specialized excipient designed to facilitate the absorption of the active drug. When semaglutide and SNAC are co-administered, SNAC transiently and locally modifies the gastric environment, creating a window of opportunity for the semaglutide molecule to pass into the bloodstream largely intact, thereby circumventing the enzymatic degradation and poor permeability that would otherwise render it inert. Without SNAC, the therapeutic efficacy of orally administered semaglutide would be profoundly compromised.
Given the critical role of SNAC in enabling oral semaglutide, researchers from the University of Adelaide embarked on the first in vivo study to systematically explore the effects of repeated exposure to this excipient. While SNAC is generally regarded as a safe compound, the study sought to investigate whether its biological impact might extend beyond simply enhancing drug absorption. Utilising an animal model over a period of 21 days, a duration chosen to simulate consistent, short-term therapeutic exposure, the scientific team meticulously monitored various physiological parameters, including the composition of gut microbiota, metabolic markers, and other indicators of overall health.
The findings, while preliminary and derived from animal subjects, revealed several notable and intriguing alterations. The research observed shifts within the gut’s microbial ecosystem, specifically identifying changes in bacterial populations that could be associated with detrimental health outcomes. The gut microbiota, a complex community of microorganisms residing in the digestive tract, plays a pivotal role in numerous physiological processes, including nutrient metabolism, immune system modulation, and even neurological function. Disturbances in this delicate balance, often referred to as dysbiosis, have been linked to a wide array of health conditions, from inflammatory bowel disease to metabolic disorders and mood disturbances. The observed changes in this crucial microbial community suggest that SNAC might not be entirely inert in its interactions with the host organism.
Concurrently, the investigation detected an elevation in specific markers indicative of systemic inflammation. Chronic, low-grade inflammation is a known contributor to the progression of various non-communicable diseases, including cardiovascular disease, diabetes, and certain neurodegenerative conditions. While inflammation is a vital protective response, sustained inflammatory states can have deleterious long-term consequences. The identification of increased inflammatory indicators in the animal models raises questions about the potential for SNAC to contribute to, or modulate, inflammatory pathways within the body.
Furthermore, the study uncovered a reduction in certain proteins known to play a role in neurological health and cognitive function. The precise implications of this depletion warrant extensive further research, but proteins involved in cognitive processes are fundamental to brain health, memory, and overall mental acuity. Any factor influencing their levels merits careful scrutiny, particularly in medications designed for long-term use.
It is crucial to underscore, as emphasized by the lead researchers, that these findings originate from animal studies and must be interpreted with caution. The results do not definitively prove that SNAC causes harm in human subjects. However, they do provide compelling evidence that an ingredient previously considered solely for its pharmaceutical-enabling properties may possess broader biological activity. Dr. Paul Joyce, a Senior Research Fellow involved in the study, highlighted this nuance, stating that while the findings do not establish human harm, they demonstrate that the excipient facilitating these tablets’ function might exert biological effects beyond its intended role in drug absorption.
The significance of these findings is amplified by the burgeoning global use of oral semaglutide. The convenience of a pill over a weekly or daily injection is a powerful driver for patient preference, promising to expand the reach of these highly effective weight loss and diabetes medications. The United States Food and Drug Administration (FDA) approved an oral version of Wegovy in late 2023, signaling a major push towards oral GLP-1 agonists. This trend, coupled with the escalating prevalence of obesity worldwide – affecting approximately 890 million adults and 160 million children, or roughly one in eight people globally – means that daily exposure to SNAC could increase dramatically. Countries like the United States and Australia, which report obesity rates of 43% and 31% respectively among adults, are witnessing a rapid uptake of these prescriptions, reflecting a broader global pattern.
Amin Ariaee, a PhD candidate at Adelaide University and lead author of the study, articulated the imperative for a holistic understanding of all drug components. He noted that while GLP-1 agonists are highly effective and are improving the lives of many individuals suffering from obesity, a complex chronic disease, the rapid expansion of oral treatments necessitates a comprehensive evaluation of every ingredient over extended periods. "As oral versions become more widely used," Ariaee stated, "we need to understand what repeated, long-term exposure to all ingredients in the pill means for the body – not just the active drug." He further elaborated that the observed shifts in gut bacteria, elevated inflammatory markers, and depleted cognitive-linked proteins, while enabling semaglutide to be taken as a tablet, clearly warrant deeper investigation.
The pharmaceutical industry typically categorizes excipients as "inactive" ingredients, primarily serving to aid in drug formulation, stability, or absorption. However, this study contributes to a growing body of research challenging the notion of complete inertness for all excipients. As medications become more sophisticated and drug delivery systems more complex, the potential for excipients to interact with biological systems in subtle, yet significant, ways becomes an increasingly important area of inquiry. This is particularly true for therapies, like those for chronic conditions such as obesity, which are often prescribed for years, if not a lifetime.
The implications of this research extend beyond the specific case of SNAC and oral semaglutide. It highlights a broader principle for drug development and regulatory science: the need for rigorous, long-term safety and efficacy assessments that encompass the entire drug formulation, not solely the active pharmaceutical ingredient. As innovative drug delivery technologies continue to emerge, ensuring patient safety necessitates a thorough understanding of how all components of a medication interact with the human body over prolonged periods. The Adelaide University study serves as a critical reminder that in the complex tapestry of pharmacological intervention, no ingredient should be presumed entirely without biological effect until comprehensively proven so. Further research, including studies in human populations, will be essential to fully elucidate the long-term safety profile of SNAC and ensure the optimal therapeutic outcomes for patients relying on these life-changing medications.






