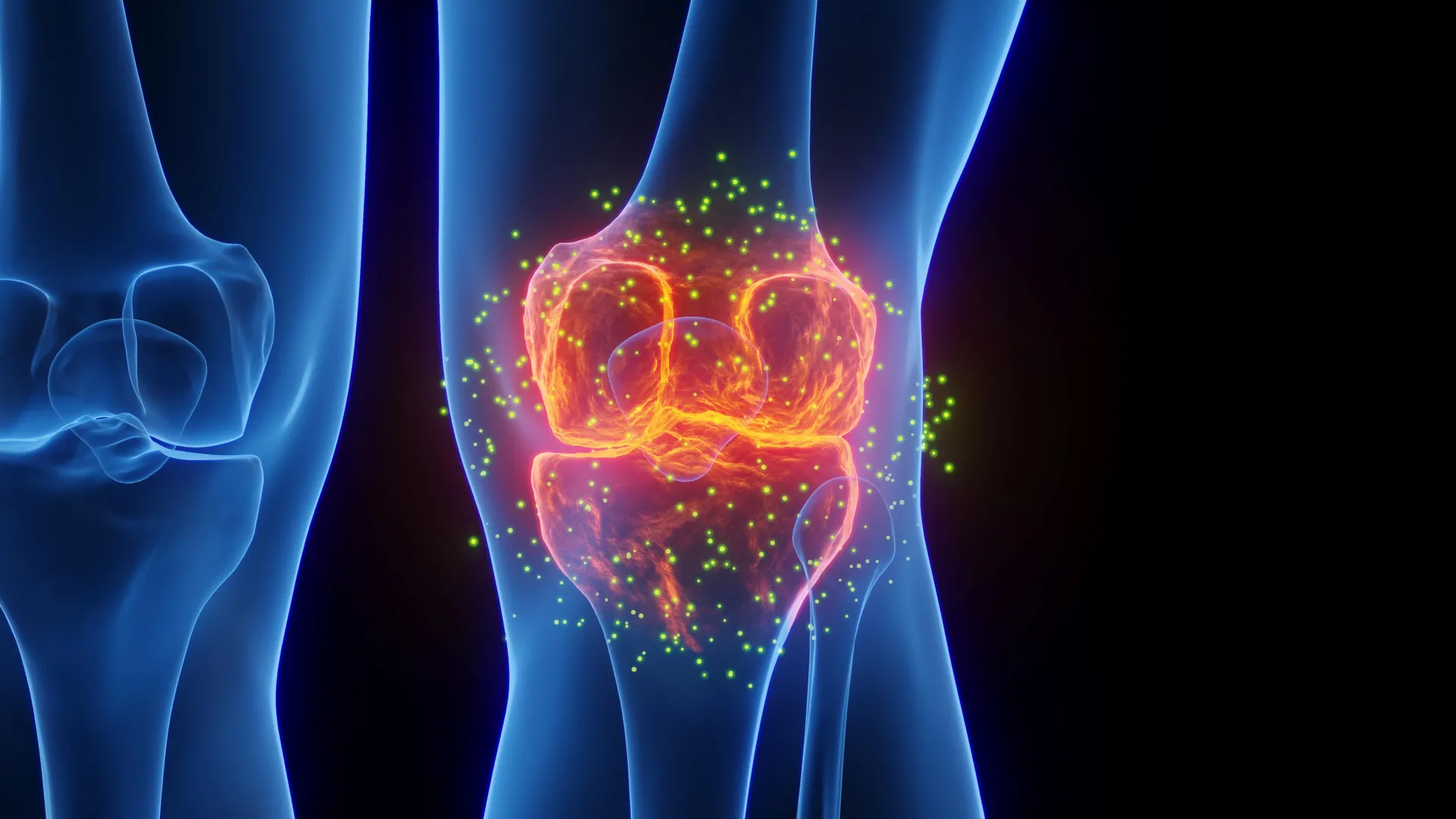
The debilitating impact of osteoarthritis, a pervasive degenerative joint disease affecting millions globally, has long presented a significant challenge to medical science. Characterized by the progressive breakdown of articular cartilage—the smooth, elastic tissue cushioning the ends of bones in joints—the condition leads to chronic pain, stiffness, and diminished mobility. Current therapeutic interventions primarily focus on symptom management, such as pain relief and anti-inflammatory drugs, or culminate in invasive surgical procedures like joint replacement when conservative treatments fail. Critically, no approved pharmaceutical agent has yet demonstrated the capacity to halt or reverse the underlying cartilage degradation that defines the disease. However, a groundbreaking study from Stanford Medicine researchers introduces a fundamentally new paradigm, suggesting that regeneration of lost cartilage and prevention of arthritis may be achievable by targeting a specific protein linked to the aging process.
This innovative research, published in the esteemed journal Science, identifies a "gerozyme" called 15-PGDH (15-hydroxyprostaglandin dehydrogenase) as a central player in age-related tissue decline, including cartilage loss. Gerozymes, a class of enzymes whose activity increases with age and drives the gradual deterioration of tissue function, were first identified by the same research team in 2023. The study’s findings reveal that blocking the activity of 15-PGDH can not only reverse the natural thinning of knee cartilage in older mice but also effectively prevent the onset of arthritis following acute joint injuries resembling anterior cruciate ligament (ACL) tears—a common precursor to osteoarthritis in humans. Furthermore, experiments conducted on human cartilage samples obtained from knee replacement surgeries showed a similarly positive response, with treated tissue demonstrating the initial formation of new, functional cartilage. This convergence of findings from diverse experimental models suggests a potent and broadly applicable strategy for combating a condition that currently imposes an estimated $65 billion annually in direct healthcare costs within the United States alone.
The implications of this discovery are profound, potentially ushering in an era where osteoarthritis is no longer an irreversible journey towards surgical intervention but a treatable condition with restorative therapies. The prospect of restoring damaged cartilage through either a systemic pill or a localized injection holds immense promise for reducing or even eliminating the need for joint replacement surgeries, thereby transforming the lives of countless individuals suffering from chronic joint pain and immobility.
The protein 15-PGDH sits at the heart of this therapeutic strategy. Its designation as a gerozyme underscores its escalating presence and detrimental influence as organisms age. Prior investigations by the Stanford team had already established a strong correlation between elevated levels of 15-PGDH in mice and a decline in muscle strength over time. Remarkably, inhibiting this enzyme using a small molecule was shown to boost muscle mass and endurance in aged animals. Conversely, genetically engineering young mice to overproduce 15-PGDH resulted in observable muscle atrophy and weakness, firmly establishing its role in age-related muscle deterioration. Beyond muscle tissue, 15-PGDH has also been implicated in the regenerative processes of bone, nerve, and blood cells, suggesting a widespread regulatory function in tissue health and repair.
A particularly intriguing aspect of the current research lies in the unique cellular mechanism observed in cartilage regeneration. While tissue repair in many other contexts, such as bone or nerve, typically relies on the activation and subsequent specialization of stem cells, cartilage appears to follow a different path. In this instance, the native cartilage-producing cells, known as chondrocytes, undergo a profound shift in their gene expression patterns. This cellular reprogramming effectively reverts them to a more youthful and regenerative state, critically, without the involvement of exogenous stem cells. This distinction marks a significant departure from conventional understandings of adult tissue regeneration and opens new avenues for therapeutic development.
Dr. Helen Blau, a professor of microbiology and immunology and director of the Baxter Laboratory for Stem Cell Biology, emphasized the novelty of this regenerative pathway. "This is a new way of regenerating adult tissue, and it has significant clinical promise for treating arthritis due to aging or injury," she stated, noting the surprise among researchers at the non-involvement of stem cells. Dr. Nidhi Bhutani, an associate professor of orthopaedic surgery, co-authored the study and highlighted the immense unmet medical need. "Millions of people suffer from joint pain and swelling as they age," Bhutani explained. "Until now, there has been no drug that directly treats the cause of cartilage loss. But this gerozyme inhibitor causes a dramatic regeneration of cartilage beyond that reported in response to any other drug or intervention."
To appreciate the significance of this breakthrough, it is essential to understand the nature of cartilage. The human body contains three primary types: elastic cartilage (found in the outer ear), fibrocartilage (dense, shock-absorbing tissue in spinal discs), and hyaline cartilage. Hyaline cartilage, also known as articular cartilage, is the smooth, glossy tissue that covers the ends of bones within synovial joints like the hips, knees, shoulders, and ankles, enabling frictionless movement. It is this type of cartilage that is predominantly damaged in osteoarthritis. The disease typically progresses as joints endure stress from aging, injury, or obesity. Chondrocytes, instead of maintaining the joint, begin releasing inflammatory molecules and breaking down collagen, the crucial structural protein of cartilage. As collagen diminishes, the cartilage thins and softens, leading to the characteristic inflammation, swelling, and pain of osteoarthritis.
A major impediment to treating osteoarthritis has been the notoriously limited regenerative capacity of articular cartilage. Unlike many other tissues, cartilage is avascular, meaning it lacks a direct blood supply, which severely hinders its ability to repair itself. While some stem or progenitor cells capable of forming cartilage have been identified in bone marrow, analogous cells have largely eluded successful identification within articular cartilage itself, further complicating repair strategies.
The journey to this discovery began with earlier research from Blau’s laboratory, which had elucidated the critical role of prostaglandin E2 (PGE2) in muscle stem cell function. They found that the enzyme 15-PGDH is responsible for breaking down PGE2. By inhibiting 15-PGDH or artificially elevating PGE2 levels, researchers had previously successfully promoted the repair of damaged muscle, nerve, bone, colon, liver, and blood cells in young mice. This led the team to hypothesize that a similar pathway might govern cartilage aging and joint damage. A comparative analysis of knee cartilage from young and old mice indeed revealed that 15-PGDH levels approximately doubled with advancing age.
Armed with this critical insight, researchers proceeded to inject older mice with a small molecule designed to inhibit 15-PGDH. The administration was performed both systemically into the abdomen and directly into the knee joint. In both experimental setups, cartilage that had become noticeably thin and dysfunctional with age exhibited remarkable thickening across the entire joint surface. Rigorous additional tests confirmed that the newly regenerated tissue was indeed functional hyaline cartilage, rather than the less robust fibrocartilage. "Cartilage regeneration to such an extent in aged mice took us by surprise," Dr. Bhutani remarked, underscoring the remarkable nature of the effect.
The team observed equally compelling benefits in a mouse model designed to mimic ACL tears—injuries frequently sustained during sports involving abrupt stopping, pivoting, or jumping. Although surgical repair can address the immediate damage, roughly half of individuals with such injuries develop osteoarthritis in the affected joint within 15 years. Mice receiving twice-weekly injections of the gerozyme inhibitor for four weeks post-injury demonstrated a significantly reduced likelihood of developing osteoarthritis. In stark contrast, control animals that received a placebo treatment exhibited double the levels of 15-PGDH compared to uninjured mice and inevitably developed osteoarthritis within four weeks. Furthermore, the treated mice displayed more normal movement patterns and placed greater weight on their injured limb than their untreated counterparts, indicating functional recovery. Dr. Blau also noted an interesting duality in PGE2’s role: "Interestingly, prostaglandin E2 has been implicated in inflammation and pain. But this research shows that, at normal biological levels, small increases in prostaglandin E2 can promote regeneration."
A more granular analysis at the cellular level provided deeper insights into the regenerative mechanism. Chondrocytes in older, untreated mice exhibited an altered gene expression profile, characterized by an increased expression of genes associated with inflammation and the undesirable conversion of cartilage into bone, alongside a reduction in genes crucial for cartilage formation. Treatment with the 15-PGDH inhibitor dramatically shifted these patterns. Specifically, a population of chondrocytes producing 15-PGDH and cartilage-degrading enzymes decreased from 8% to 3%. Another group of cells linked to fibrocartilage formation declined from 16% to 8%. Concurrently, a third population of chondrocytes, which did not produce 15-PGDH and instead expressed genes vital for hyaline cartilage formation and the maintenance of the extracellular matrix, surged from 22% to 42%. These profound changes collectively point towards a broad reversion to a more youthful and healthy cartilage profile, achieved through the reprogramming of existing cells rather than the introduction or activation of stem cells.
Crucially, the researchers extended their investigations to human cartilage samples obtained from patients undergoing total knee replacement surgery for osteoarthritis. After just one week of treatment with the 15-PGDH inhibitor, the human tissue samples demonstrated fewer 15-PGDH-producing chondrocytes, a reduced expression of genes associated with cartilage degradation and fibrocartilage formation, and early, encouraging signs of articular cartilage regeneration. Dr. Bhutani concluded, "The mechanism is quite striking and really shifted our perspective about how tissue regeneration can occur. It’s clear that a large pool of already existing cells in cartilage are changing their gene expression patterns. And by targeting these cells for regeneration, we may have an opportunity to have a bigger overall impact clinically."
The path forward now turns towards human clinical trials. Dr. Blau highlighted that Phase 1 clinical trials for a 15-PGDH inhibitor targeting age-related muscle weakness have already established its safety and activity in healthy human volunteers. This existing data could significantly accelerate the development timeline for a cartilage-focused therapy. "Our hope is that a similar trial will be launched soon to test its effect in cartilage regeneration," Blau articulated, expressing palpable excitement for this potential breakthrough. "Imagine regrowing existing cartilage and avoiding joint replacement."
This monumental research received support from various prestigious institutions and funding bodies, including the National Institutes of Health, the Baxter Foundation for Stem Cell Biology, the Li Ka Shing Foundation, and the Stanford Cardiovascular Institute, among others. It is also important to note that Dr. Blau, Dr. Bhutani, and other co-authors hold inventor status on patent applications related to 15-PGDH inhibition in cartilage and tissue rejuvenation, which are licensed to Epirium Bio. Dr. Blau is also a co-founder of Myoforte/Epirium and possesses equity and stock options in the company, reflecting the direct translational potential of this scientific endeavor. The collaboration with researchers from the Sanford Burnham Prebys Medical Discovery Institute also contributed significantly to the study’s comprehensive findings. This multi-faceted effort underscores the rigorous scientific foundation and the clear translational vision behind a discovery that could fundamentally reshape the landscape of osteoarthritis treatment.





