A groundbreaking international scientific collaboration has brought to light a previously unappreciated immunological function for human serum albumin, the most abundant protein found in circulating blood. This ubiquitous protein, long recognized for its roles in maintaining osmotic pressure and transporting various molecules, now stands revealed as a potent, natural protector against mucormycosis, a rare but frequently lethal fungal infection. The pivotal findings, detailed in the prestigious journal Nature, were spearheaded by Dr. George Chamilos and his research team at the University of Crete and the Institute of Molecular Biology and Biotechnology in Greece, with significant contributions from Professor Ashraf Ibrahim’s group at The Lundquist Institute for Biomedical Innovation in the United States. This discovery offers a profound re-evaluation of the body’s intrinsic defenses and opens promising new avenues for diagnosing and treating this aggressive disease.
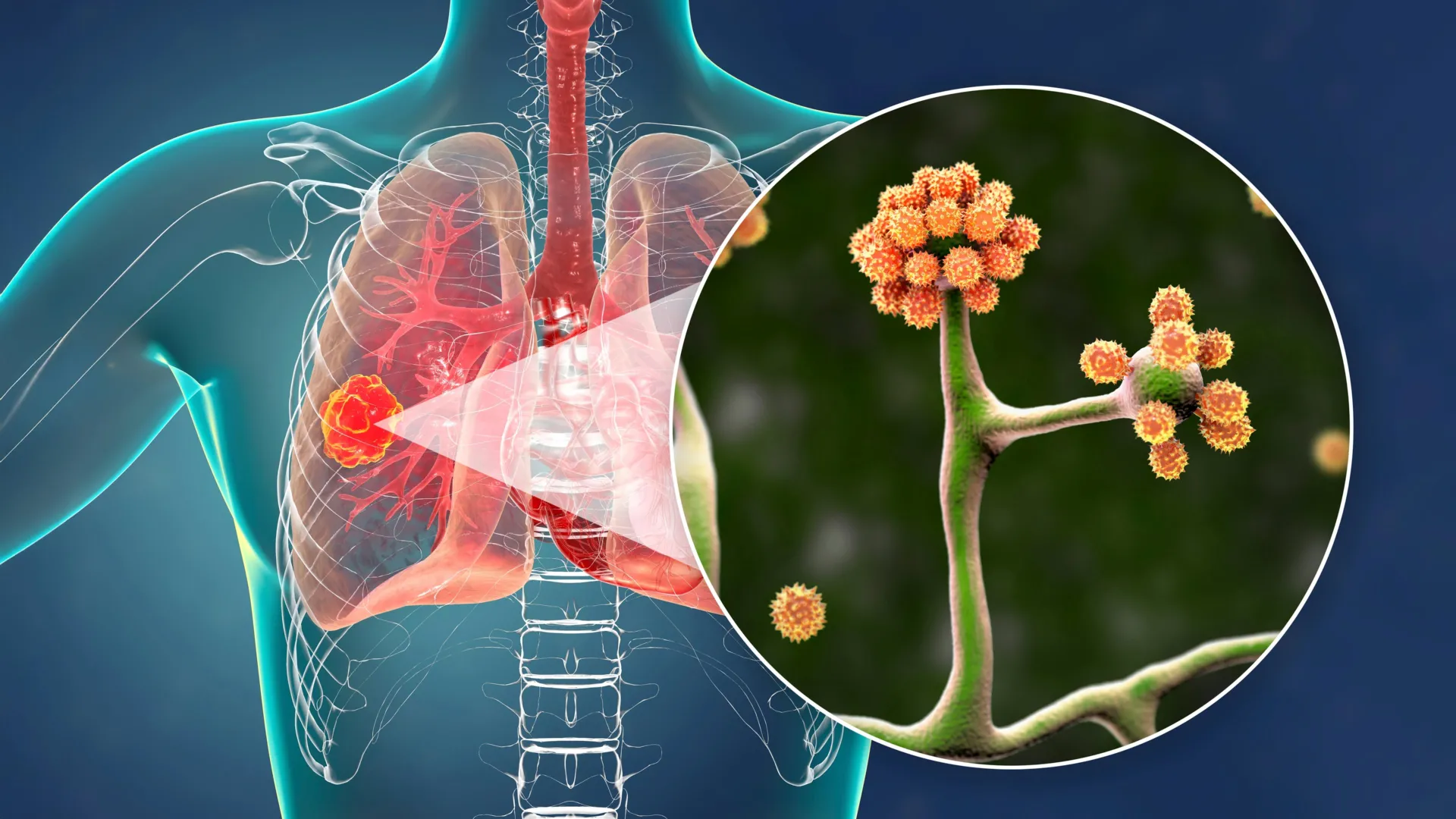
Mucormycosis, colloquially known as "black fungus," is an opportunistic infection caused by fungi belonging to the order Mucorales. These ubiquitous molds, found in soil, decaying organic matter, and even airborne spores, typically pose little threat to healthy individuals. However, in those with compromised immune systems, uncontrolled diabetes, malnutrition, or other underlying health conditions, they can rapidly proliferate, invading tissues and organs. The infection’s devastating progression is characterized by rapid spread, often necessitating extensive surgical debridement alongside antifungal medications, yet it still carries an alarmingly high fatality rate, approaching 50% in many cohorts and even higher in specific patient populations. The global medical community witnessed a stark and tragic illustration of mucormycosis’s virulence during the COVID-19 pandemic, particularly in India, where a surge in cases was observed among individuals recovering from the viral illness, frequently exacerbated by pre-existing diabetes or the use of corticosteroids. The urgent need for more effective diagnostic tools and therapeutic interventions for this dire condition has never been more apparent.
The research team’s initial investigations into mucormycosis patients yielded a striking observation: individuals afflicted with the fungal infection exhibited significantly diminished levels of circulating albumin compared to patients battling other types of fungal infections. This condition, medically termed hypoalbuminemia, emerged as an exceptionally strong prognostic indicator. Across diverse patient populations spanning multiple continents, lower albumin concentrations consistently correlated with more severe disease progression and a heightened risk of mortality. This finding is transformative, as Dr. Ibrahim, a senior author on the study, remarked, suggesting the potential to fundamentally alter clinical approaches to managing mucormycosis. Identifying hypoalbuminemia could serve as an invaluable biomarker, enabling clinicians to pinpoint individuals at elevated risk of succumbing to this rapidly advancing infection, thereby allowing for earlier, potentially life-saving interventions. Furthermore, the study hints that therapeutic administration of albumin, particularly formulations enriched with free fatty acids, could play a preventative role, curtailing the infection’s ability to establish itself—a crucial strategy given mucormycosis’s swift and destructive trajectory.
Beyond mere correlation, the study meticulously delved into the mechanisms by which albumin exerts its protective effects. Dr. Ibrahim further elaborated that the research elucidated how albumin directly counteracts critical virulence factors deployed by Mucorales fungi. These factors include toxins and various fungal proteins that are instrumental in causing tissue damage and aggressively invading human organs. The insights gained into these molecular interactions not only deepen our understanding of innate immunity but also pave the way for novel therapeutic designs. For instance, the possibility now exists for combining albumin-based treatments with targeted immunotherapies specifically engineered to disarm Mucorales virulence factors, an area of active investigation by researchers at The Lundquist Institute.
Rigorous laboratory experiments provided compelling evidence for albumin’s specific antifungal properties. In vitro assays demonstrated that albumin selectively inhibited the growth of Mucorales fungi without adversely affecting other microbial species, underscoring its precise action. When albumin was deliberately removed from healthy human blood samples, the pathogenic fungi multiplied unimpeded, flourishing in the absence of this crucial protein. The researchers further corroborated these findings through in vivo studies using animal models. Mice genetically engineered to lack albumin displayed a marked vulnerability to mucormycosis infection, succumbing more readily to the pathogen. Conversely, the restoration of albumin levels in these susceptible animals conferred substantial protection against the fungal challenge, unequivocally establishing albumin’s direct role in host defense.
A deeper dive into the biochemical intricacies revealed that albumin’s potent antifungal activity is intrinsically linked to the fatty acids bound to the protein. These fatty acids are not merely passengers but active participants in the defensive mechanism. They interfere with vital fungal metabolic pathways, effectively disrupting the pathogen’s ability to synthesize proteins essential for tissue invasion and disease progression. This discovery adds another layer of sophistication to albumin’s multifaceted biological roles. Intriguingly, blood samples obtained from patients suffering from mucormycosis exhibited elevated levels of fatty acid oxidation. This phenomenon could potentially deplete the pool of fatty acids available to bind with albumin, thereby diminishing the protein’s antifungal capacity and contributing to the patients’ heightened susceptibility to the infection.
Collectively, these comprehensive findings illuminate a previously unrecognized, yet fundamental, natural defense mechanism within the human physiological framework. The revelation that a common blood protein like albumin possesses such potent, specific antifungal capabilities against a notoriously difficult-to-treat pathogen represents a paradigm shift in our understanding of innate immunity. Furthermore, the implications for clinical practice are profound. The identification of hypoalbuminemia as a powerful biomarker could enable earlier diagnosis and risk stratification, leading to more timely and aggressive interventions. More critically, the research strongly suggests that albumin-based therapies, particularly those utilizing albumin enriched with specific fatty acids, could furnish a much-needed, innovative approach to both preventing and treating mucormycosis. Given the current limitations in effective treatment options for this devastating disease, the prospect of leveraging an intrinsic bodily component as a therapeutic agent offers a beacon of hope for improving patient outcomes and significantly reducing the morbidity and mortality associated with "black fungus." This scientific endeavor not only expands the frontiers of immunological knowledge but also promises tangible benefits for patients worldwide confronting this formidable fungal threat.